Creating a Patient Monitoring System
Scalable digital solution connecting hypertensive patients and nursing teams in a managed care environment.
Context
Medicinia
Health-tech startup focused on safe, human-centered communication between healthcare companies, physicians and patients.
MOPE
Special Patient Monitoring Team (MOPE in Portuguese). Nursing team dedicated to remotely monitoring patients from the health insurance company São Cristóvão Saúde (based in Brazil).
Problem
Business Problem
The MOPE Team needed to increase patient coverage without increasing nurse workload or clinical risk using a digital solution as a way to expand and enhance its reach, capacity and quality of care.
Business Need
Align product scope with clinical constraints, operational capacity, and measurable outcomes for remote hypertension programs.
User Problem
Nurses needed workflows that reduced cognitive load during remote follow-ups while keeping patients engaged between in-person visits.
User Need
Clear, timely communication channels and lightweight tasks patients could complete without friction on common devices.
Why was this important?
As patient volume increased, the monitoring team could not scale manual follow-ups without compromising care quality and nurse workload.
Goal
Provide safe, scalable, and engaged care for nursing teams monitoring hypertensive patients beyond traditional follow-ups.
Research & Insights
Understanding the problem
To understand the context, exploratory conversations were conducted with the monitoring team (team leaders, nurses, and attendants) to learn how patient monitoring was currently performed, the challenges faced, and unmet needs.
For patient context, the MOPE team helped to select patients that could be part of the pilot solution.
Research
Research focused on understanding existing monitoring workflows, patient engagement, tracked health indicators, data organization, and communication during follow-up. In parallel, we reviewed the hypertension care protocol to identify the key events and indicators that would guide the solution.
Key Insights
- Nurses relied on informal tools (WhatsApp, spreadsheets) to track patients
- Different indicators required different urgency levels
- Patients had difficulty maintaining daily routines without reminders
Key Outcomes
Health Indicators
- Quarterly specialist consultations
- Semiannual secondary specialist consultations
- Daily blood pressure monitoring
- Daily medication adherence tracking
- Monthly weight monitoring
MVP Premises
- Patients who already use smartphones on a daily basis.
- Follow indicators and frequency of measurements set on the Hypertension Protocol of the Brazilian Society of Cardiology.
Solution
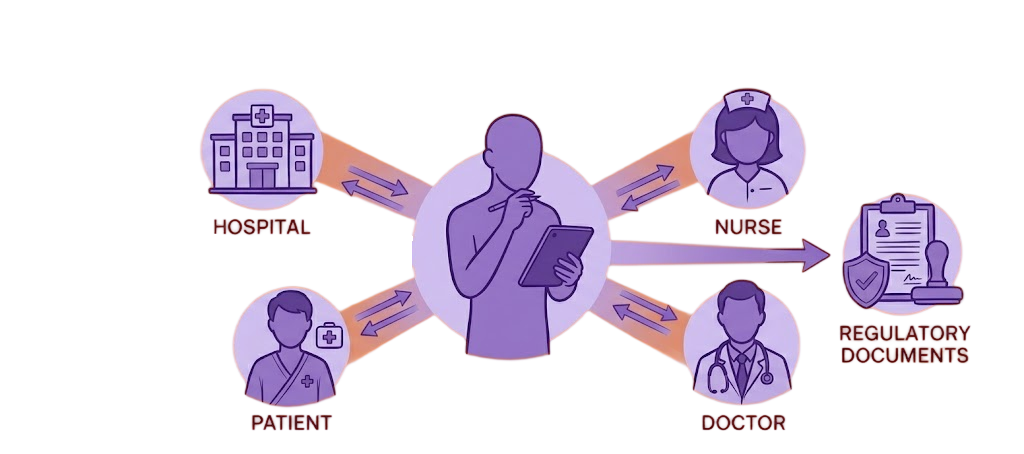
The solution combines structured indicator tracking, multi-channel patient communication, and a nurse-first monitoring workspace—so teams can act on the right signal at the right time.
Monitoring indicators and patient contact channels
Based on the type, relevance, and frequency of each health indicator, I pushed for defining the most appropriate patient communication channels—chat, alerts, tasks, orientation messages, and phone calls—ensuring data was exchanged in the right context and could be acted on effectively by nurses and the system.
Patient Tracking — Overview
Nurses get a prioritized view of patients, recent indicators, and open conversations in one place—reducing tab-hopping between informal tools during follow-up.
Segmented Patient Onboarding
Because the number of required indicators and explanations directly affected patient adherence, onboarding was intentionally distributed across multiple moments during the first week of app use. This approach reduced cognitive load while introducing information in context with each monitoring event.
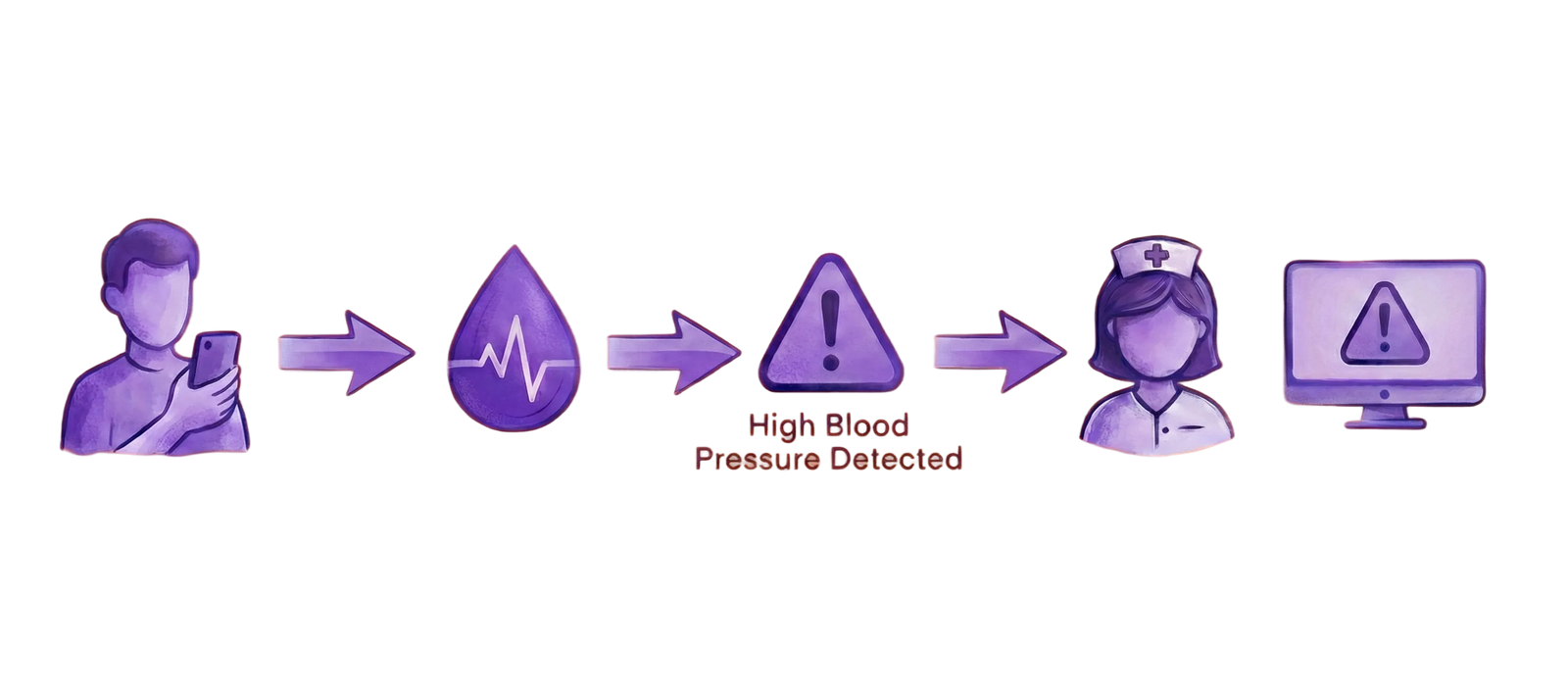
Monitoring Team View — Alerts for Critical Indicators
For the MVP to be effective, the monitoring team needed immediate access to patient-entered indicators, as well as timely alerts when values fell outside defined clinical thresholds (for example, blood pressure readings that were too high or too low). To support this, I advocated for contextual alerts and data triggers that provided nurses with a clear, objective view of patient data throughout the monitoring period, enabling faster recognition of risk and appropriate clinical response.
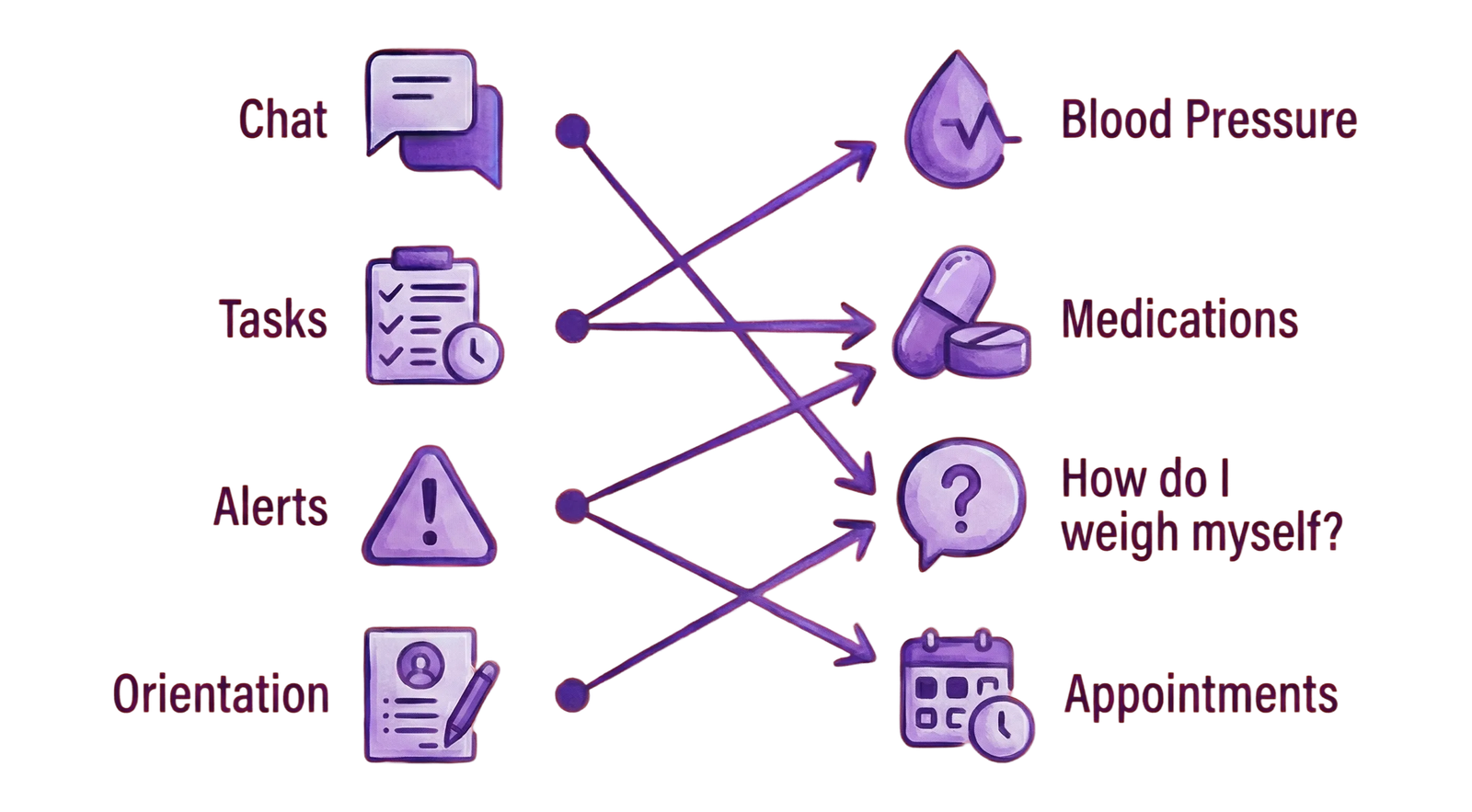
Channels × Indicators
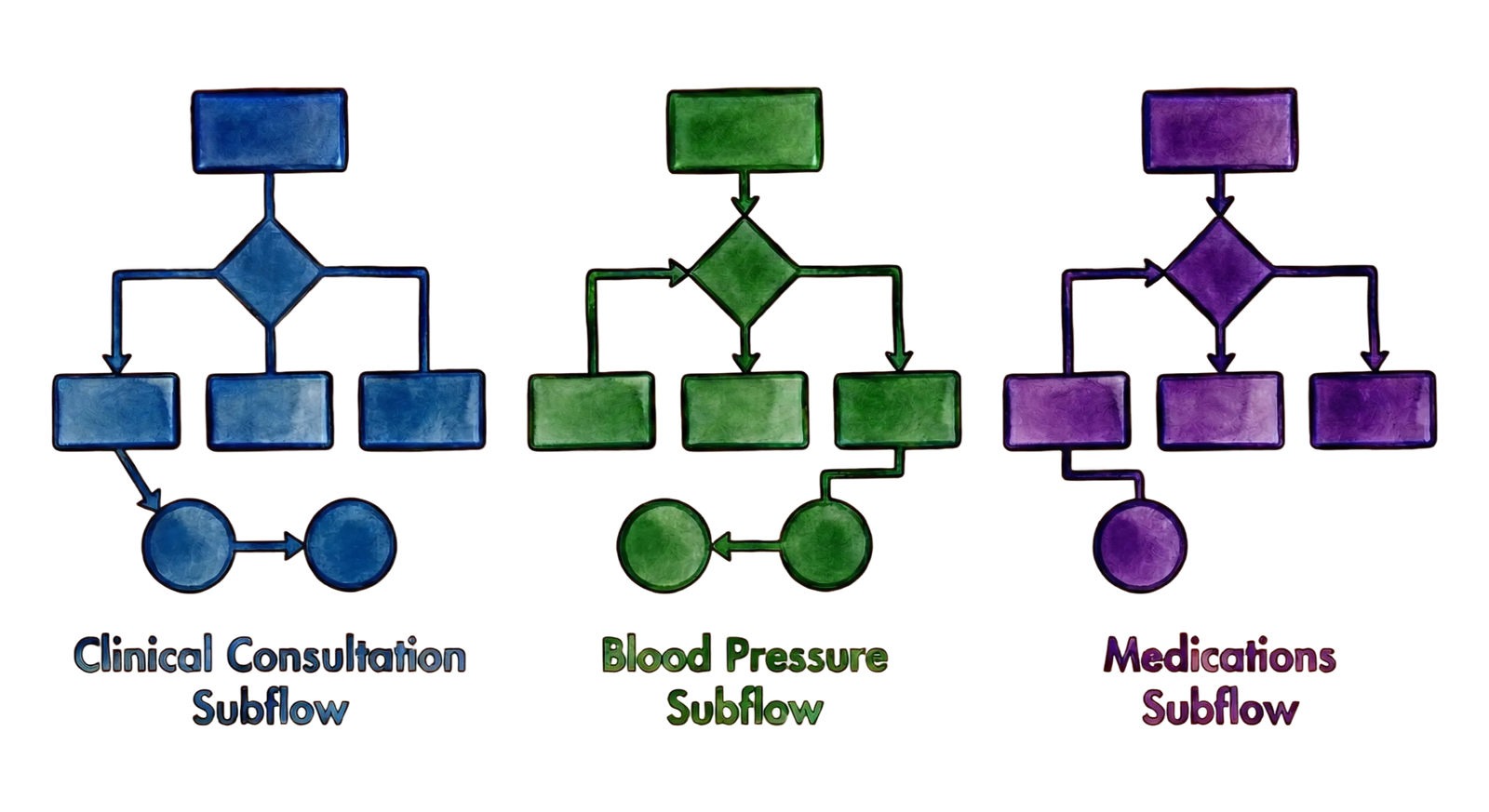
To support different monitoring needs, individual flows were defined for each health indicator, combining the most appropriate communication channels and content types. Together, these flows form a modular system structure that allows monitoring logic, frequency, and responses to adapt to each indicator’s context.
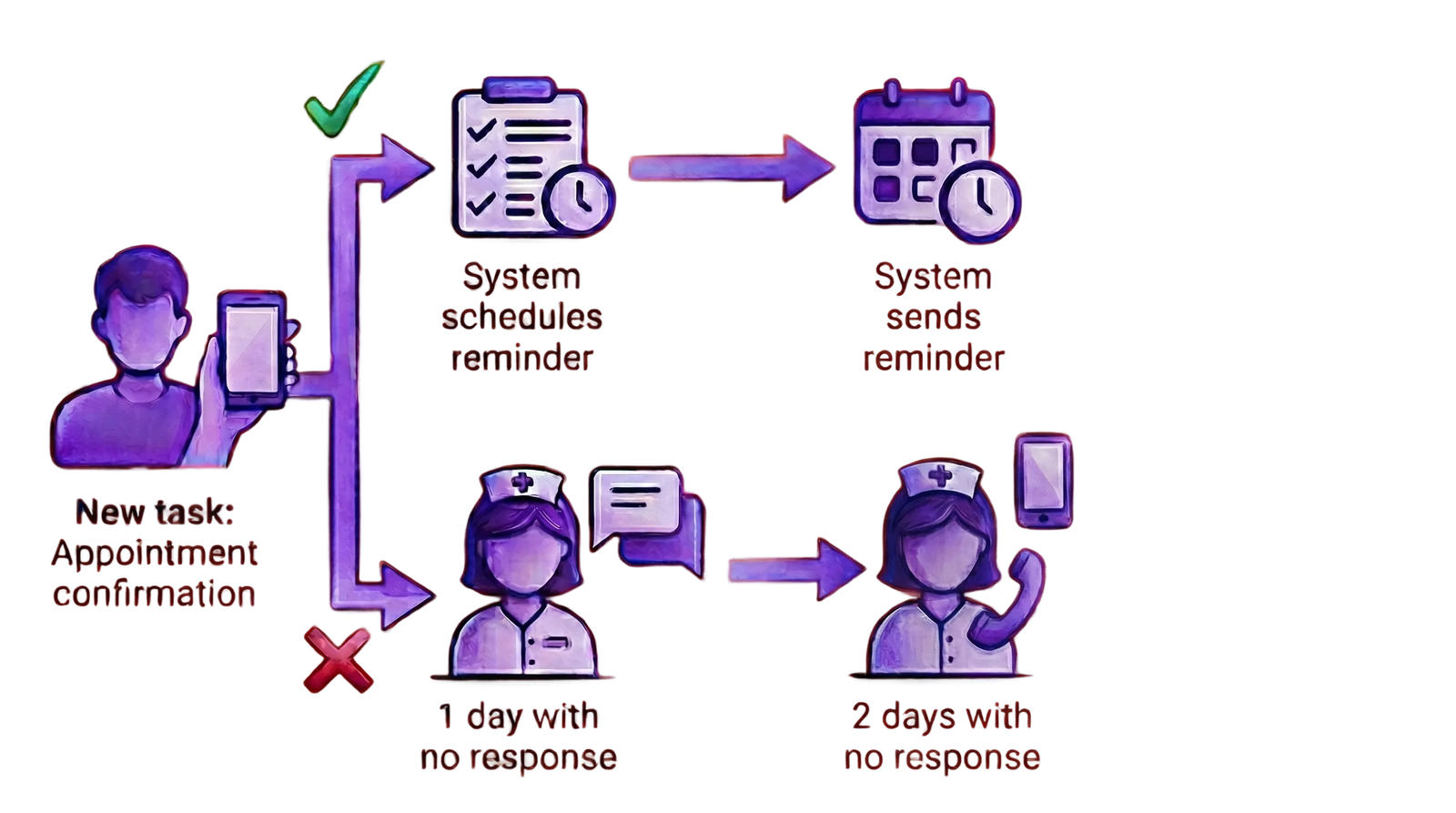
Subflow Example
Example flows show how a single indicator triggers the right sequence of tasks, messages, and escalations—so patients and nurses stay aligned on what happens next.
Distributed Onboarding
This approach delivered the following benefits:
- Patients received tasks and orientations only when relevant to their monitoring stage.
- Early cognitive load was reduced by avoiding multiple tasks or large data entry during first use.
- Patients were gradually introduced to the monitoring ecosystem, improving understanding and long-term adherence.
Mockups & User Flow
Flow
The end-to-end flow connects patient tasks, nurse chat, and escalation paths so teams can follow a single journey from first contact through resolution.
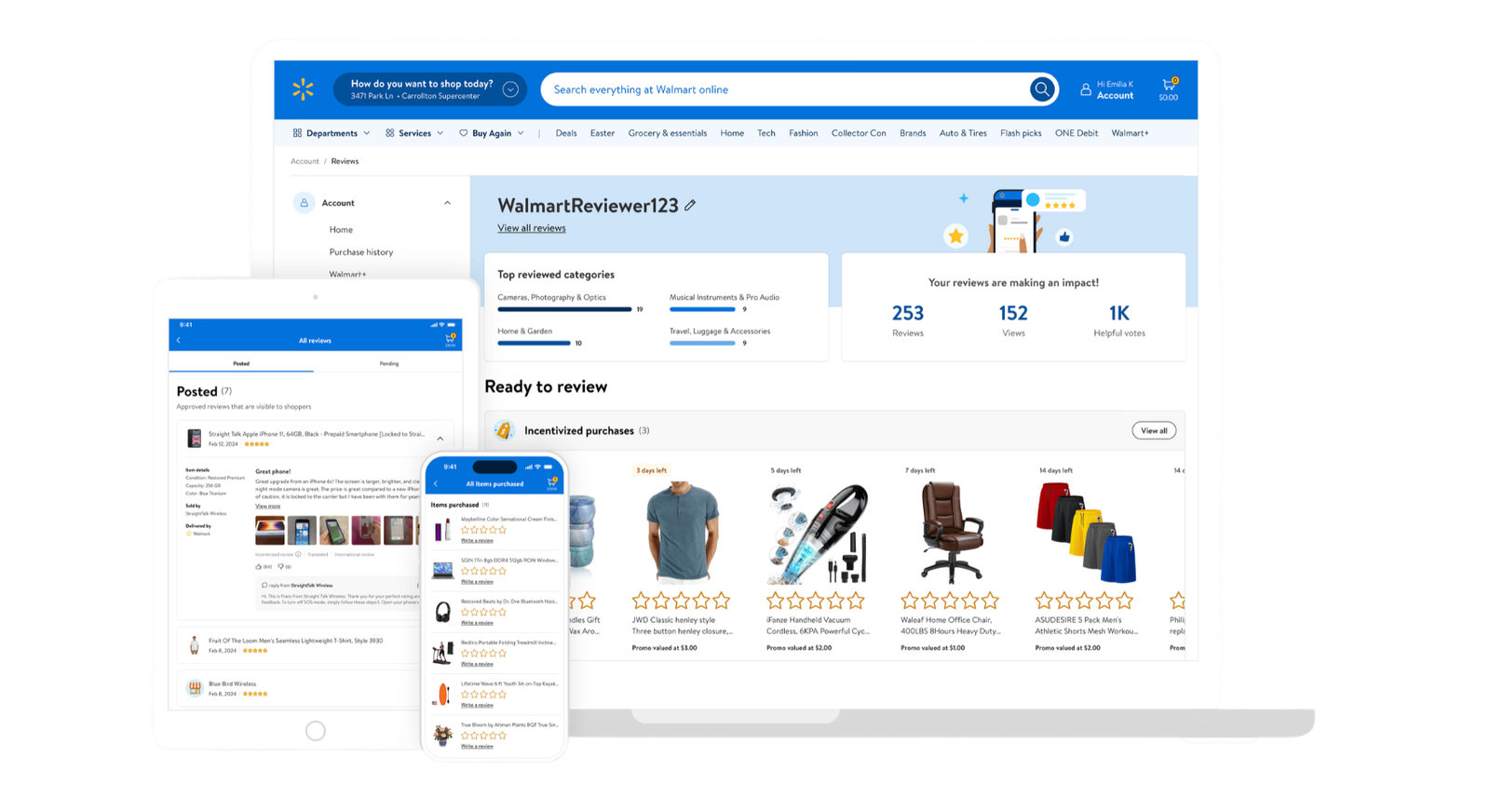
MOPE System
The MOPE web workspace brings together patient lists, real-time messaging, and clinical context in one place—aligned with how nurses monitor cases today.
Key Strategic Decisions
Accelerating learning through Web View
To maximize learning speed during early validation, patient-facing screens were implemented using Web Views instead of native components. This decision significantly reduced deployment friction, allowing the team to iterate on UX, content, and interaction patterns without repeated app store releases and enabling faster response to insights from testing.
Designing for change with a flexible backend
I collaborated closely on the definition of the backend data model, advocating for a generic and extensible structure. This approach allowed indicators, flows, and clinical protocols to evolve over time without major structural changes, supporting both scalability and long-term product adaptability.
Validating workflows before automation
Rather than automating processes prematurely, early testing relied on manual triggering of tasks and alerts, with the monitoring team acting as test patients. This deliberate choice prioritized understanding real workflows and refining UX and system logic before committing to automation, reducing downstream rework and risk.
Modeling for evolution
Advocating for a generic backend model involved close collaboration with engineering to balance short-term delivery pressure with long-term flexibility.
The indicator-based flow model established a reusable foundation that could support additional conditions beyond hypertension without redesigning the system.
Summary
Two complementary surfaces
Indicator-specific subflows connect these two components through patient data entry and system events. Together, automated responses and nurse interpretation form a unified monitoring flow that supports continuous, safe patient follow-up.
Accelerating learning through embedded web view
The solution can be understood as two complementary components:
- Tools for the monitoring team including:
- Chat,
- Alerts for critical indicators (such as abnormal blood pressure or weight), and
- Easy access to patient data.
- A patient-facing app with chat, tasks, alerts, reminders, and educational content to support daily monitoring.
Outcomes & Learnings
Outcomes
- Delivered a modular monitoring MVP aligned with clinical protocols and real nurse workflows.
- Enabled safe scaling by combining automated alerts with nurse interpretation instead of a single linear process.
- Improved patient comprehension and adherence through progressive onboarding and contextual communication.
- Provided nurses with a unified view of patient communication and recent indicators, reducing cognitive load during follow-up.
Key Learnings
- Adherence depends on timing, not volume: distributing indicators and guidance over time reduced friction and confusion.
- Clinical monitoring requires modularity: decoupling channels and content allowed each indicator to define its own flow.
- Automation supports (but does not replace) clinical judgment: alerts were most effective when paired with context and human analysis.
- Healthcare UX is systems design: small interaction decisions can significantly impact safety, workload, and trust.